Formula 1 and its Contributions to Healthcare
Share
- Details
- Text
- Audio
- Downloads
- Extra Reading
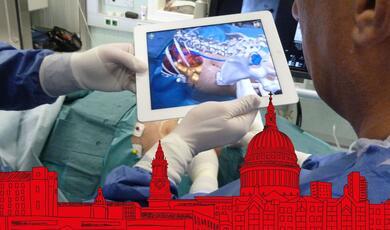
At first sight, there is little relationship between the high tech, high cost, high speed and highly competitive world of F1 and heart surgery for children. Yet Formula 1, with its extraordinary teamwork, rates of innovation, commitment to excellence and relentless pursuit of safety has taught us a great deal.
This lecture will consider the parallels between our activities, describe the lessons learned and consider how we, in healthcare, might benefit more from how they work and their technology. And a little of what they have learned from us!
This lecture is a part of Biology Week 2015.
Download Text
14 October 2015
Formula 1 and its Contributions to Healthcare
Professor Martin Elliott
Humans have always been attracted to danger and speed, and love to race; you only have to think of the chariot racing sequence in Ben Hur. Hence Formula 1; but Formula One is brash, wasteful, often misogynistic, expensive, and remains politically, financially and socially controversial. Yet it is glamorous; dangerous and exotic, attracting a global audience especially the rich and famous, and it provides a media circus all of its own.
It is not surprising that modern F1 drivers have been likened to the gladiators of old. Even for the crowd, an F1 race it is a visceral experience, but for a driver it is something else. As Jenson Button has put it, "To understand the intensity of driving an F1 car, you have to be in it. When you're driving a 750hp machine at 200mph, the noise and the vibrations are incredible. The G-force when you take big corners is like someone trying to rip your head off. You hit the brakes, and it feels as if the skin is being pulled off your body." But apart from having your skin ripped off (which sounds pretty medical), what on earth has Formula One got to do with healthcare, and how can it possibly have made any real contributions to our work? Well it has helped us in five key domains; teamwork, safety, rapid prototyping, big data analytics and logistics.
I want to start by telling you the story of how my unit, The Cardiac Unit at The Great Ormond Street Hospital for Children, became involved with the people of F1, and what we have learned since. It is a story of honesty, curiosity, exploration, research and sharing. And it highlights key similarities (and differences) between my world of paediatric heart surgery and that of F1. There turned out to be lessons for all of us.
When Sir Ian Kennedy delivered his Bristol Inquiry Report in 2001, one of the things he highlighted was the danger associated with the transfer of a child from the cardiac operating rooms to intensive care. Although not explicitly covered by his report, there were good reasons why this apparently simple journey should be so risky. I want to take you on that journey to explain why.
Any child has to be prepared very carefully to undergo such surgery and be made safe within the extremely complex environment of the operating theatre. The diagnosis must be right, everybody must be certain of what operation is going to be performed and what their individual role is going to be, and all the relevant equipment must be available and working.
The baby must be anaesthetized, provided with intra-venous and intra-arterial lines to measure pressures and give fluids, connected to devices that monitor ECG, temperature and oxygen saturation. She must be catheterized to monitor urine output and placed on a heated mattress to help control temperature. Only then can the child be prepared for the actual incision itself.
Once the child is in the operating room, the skin must be cleaned and sterilized with antiseptic solution, which is allowed to dry. The area where the incision is to be made is isolated by sterile adhesive drapes and sealed with an adhesive iodine impregnated plastic layer to minimise the risk of infection. The child is covered, with only the area of the incision visible to the surgeon. Perhaps surprisingly, the anaesthetist also can only see a tiny amount of the baby, so it is vital that all the lines, wires and connectors are carefully positioned and safe. The child is essentially in a ' drive by wire' state, with many physiologic variables being monitored continuously and displayed on TV screens, visible to all.
Despite this logical state, the whole picture can appear one of chaos, with wires and tubes appearing like a complex set of knitting. The potential for error is enormous; just tripping over a line could be catastrophic. But thankfully the child in the care of a dedicated team of up to 25 people, each individual devoted to her wellbeing.
Many cardiac operations take a long time, at least half a day. During the procedure, the team will have to give fluids such as blood or saline in varying volumes, and a variety of drugs in different doses calculated to the microgram per kg body weight. Each of these interventions will invoke a response from the child in terms of the variables being monitored, e.g. arterial and venous pressures, saturations and urine output. Each child is different, and responds differently to the interventions. Their physiology is unique.
So, over the course of the several hours of surgery, the team (and especially the anesthetist and surgeon) will develop a pretty deep understanding of how that particular child behaves and what the consequences of any intervention might be. You really get to 'know' the child. But, because of its subtlety, this understanding can be very hard to communicate.
At the end of the operation, after the wound is closed and the drapes removed, the child is ready for transfer back to the intensive care ward. But it has to be made ready for the journey, and that is not as straightforward as it sounds.
Firstly, the trolley must be brought to the side of the operating table. The trolley is not heated, so the baby, who has been maintained warm and cosy for so long, is suddenly transferred to a cool and harsher environment. Secondly, all the syringe pumps, which have been powered from mains AC current during the operation, have to be switched to DC current via battery power and be moved onto the trolley, without tangling all the pipes. Similarly, the monitoring equipment must be transferred, again without tangle.
Finally, the child must be disconnected from the mechanical ventilator to which it has been accustomed over some hours, and the anesthetist must 'hand bag' the child during the journey. This is important. It is really easy to alter the dynamics of both air and blood flow through the lungs by changing the how hard and how often you squeeze the bag. This can have a major impact on the baby's heart by altering the resistance to blood flow through the lungs
An operation note and an anaesthetic chart accompany the baby back to the ward, but a great deal of more detailed information about how the baby 'works' is, by default, held in the combined brains of the team. The team members are often pretty tired, are keen to speak to the baby's parents and probably want to go home after a long day.
The baby is then pushed down a corridor (and may be up or down floors in an elevator), surrounded by key staff, to arrive in the ICU, and to be met by a team which cannot yet know the baby, nor how it works. That new team needs to understand all of this because they are going to look after the child for several critical hours, often the most critical.
All the monitoring, drugs and plumbing must be reconnected, including to AC current, mechanical ventilation and so on, and an attempt must be made to transfer all the relevant knowledge, as the surgical team returns for the next case or to leave. The receiving ICU team has both to assimilate that knowledge and feel able to undertake all the changes to care that might be necessary.
It is not surprising that transfer and handover errors were common. They were errors of omission (forgetting to do something or pass on some vital piece of information) or commission (doing the wrong thing, or passing on the wrong information). Accurate handover and appropriate use of common terms is critical.
Such errors were not limited to Bristol. In a landmark study 1 designed by my renowned predecessor at Great Ormond Street, Professor Marc de Leval, similar observations were made by Dr. Jane Carthey, a psychologist who travelled the country observing in each of the cardiac centres the arterial switch operation in neonates, looking for any human factors which might influence outcome. Wherever she looked, the transfer from theatre to ICU was fraught with danger, inconsistency and poor communication.
Team dynamics and personalities clearly play a role in this. Surgeons are notoriously impatient and irascible, and often poor communicators, particularly after several hours of intense focus. Historically, they have tended to dominate conversations and expect things to be done 'their way'. And they have not been great at either listening to others or working to standard operating procedures. In addition, at the end of a long operation they are, frankly, tired. Not really a good set up for perfect communication.
We had been worrying about this problem of the patient transfer for some time, but one Sunday in the mid-noughties, after a night up doing a heart transplant and then a complex neonatal operation in the morning, I was sitting with my intensive care colleague, Allan Goldman, watching the Formula 1 Grand Prix on TV; we seem to remember from Barcelona in Spain. The racing was good and mind emptying after such a lot of work, but suddenly a McLaren came into the pits to refuel and get a new set of tyres; all done in a few seconds. The camera angle chosen by the director showed the positioning of their multidisciplinary team, the things that needed to be done to the car and the sheer professionalism of the process. The car had come in, various components were disconnected and reconnected by a dedicated team of people, information was exchanged with the driver and data forwarded to the pit wall. All the tasks done were carried under huge time pressure, and in public.
We looked at these images and realised that there was no fundamental difference between what they do in the pit stop and what we do in a patient handover. They were managing hardware and software and transferring information. Just as we do. That realization prompted us into action. We were lucky enough to have working in our unit the son of Sid Watkins, the senior F1 doctor, and as a result Sid senior put us in touch with McLaren. The McLaren team was interested and within a few days Dave Ryan came to GOSH to explain pit stops to us and to see how they could help. There was an immediate chemistry and recognition of both differences and similarities between our worlds. Sadly, we couldn't get funding to do the work, but thanks to a management training day with Shell, we were introduced to the Ferrari team, whose guests we were at Silverstone to watch pit stop rehearsals with Ross Brawn and the late Nigel Stepney. The research team went to Maranello, the home of Ferrari to develop the project with Nigel Stepney. He was not impressed by what we were doing. As our lead researcher Dr. Ken Catchpole recalled later when interviewed by the Wall Street Journal, Stepney was "amazed at how clumsy and informal the hospital handover was". With Ferrari's help we managed to get a grant from the Department of Health and the Institute of Child Health at UCL
As I will show you…things got better, and we were able to prove that in another landmark study 2 led by Ken Catchpole and Annette McQuillan and funded by the Patient Safety Research Programme of the Department of Health, UK and ICH.
I want to explain what is special about a pit stop, what Stepney identified as bad about what we were doing, and what we did to change things. There were safety and performance themes that were embedded in F1 culture, which we had to adapt. These were:-
Leadership; in those days of F1, the 'lollipop man' coordinated the pit stop and was in effective control. In our old practice, it was unclear who was in charge – at any phase in the process. In the new process, the anaesthetist was in charge of coordinating the whole thing, handing over formally to the intensivist only at the end of the handover.
Task Sequence; in F1 there is a clear rhythm to events. Our old method was inconsistent (each team did the handover a bit differently) and non sequential. In the new handover, the process was split into three logical phases
1.Equipment and technology handover (making sure you could see how the baby was and maintaining life support) 2.Information Handover (what is wrong, what was fixed, and what was learned) 3.Discussion and Plan (get ready for the next few hours)Task Allocation; in F1each team member has only one or two carefully defined tasks. Our old system was erratic and informal; everyone tried to help, (hardly surprising really because that is why most of us joined up in the first place). In the new system, the ventilation was managed by the anaesthetist, the monitoring by the ODA, and the drains by the nurses. The anaesthetist also defined any additional roles.
Predicting and Planning; F1 used a formal Failure Modes and Effectiveness Analysis (FMEA) to define both tasks and risks. In our old system, whilst risks were identified, the process was informal and risks were often not acted upon. In the new arrangements we carried out FMEA, with the senior staff commenting on areas of high risk. Additional safety checks on equipment were introduced and a ventilation transfer sheet created, initiated before the transfer took place.
Discipline and Composure; There is very little verbal communication during an F1 pit stop. In our old system, there were plenty of conversations and these were ad hoc and unstructured, and often several took place simultaneously. Now, communication is limited to the essential whilst equipment is sorted out, and then each party speaks in turn, followed by discussion and planning.
Checklists; Checklists are integral to the way F1 works. They did not exist for medical handover before this work, and are now mandatory documents in our new system.
Involvement; in F1 members of the team are actively encouraged to speak up, especially during training. In our old practice, old-fashioned hierarchies often prevented juniors from speaking if they observed something which, in their view, posed a risk. Now they and all members are encouraged to speak up.
Briefing; F1 has well-established culture of briefing for the pit team, even on race day. We had such a system, but it was pretty basic and had to be refined.
Situation Awareness; the 'lollipop man' or modern equivalent has oversight over the whole pit stop process, ensuring that the team is aware of what is going on around them, if required. In our handovers, this was not considered important in the old days, but now the consultant anaesthetist and intensivist take on that role and regularly step back to check all is OK; keeping an eye on the bigger picture.
Training; F1 has a fanatical approach to training and repetition. We had no handover training until this work. Our new process could be learned in 30 mins, and now is part of induction of all new staff, who 'turn over' frequently.
De-briefing and review meetings; F1 had regular team meetings to review performance. We had a weekly meeting in place, which became a venue to discuss handover issues.
Nigel Stepney was not impressed by what we were doing. As Ken Catchpole recalled later when interviewed by the Wall Street Journal, Stepney was " amazed at how clumsy and informal the hospital handover was".
These don't seem like big things, but the development of a
clear structure, and a choreographed standard operating procedure - repeatedly rehearsed - had a significant impact. We were able to reduce technical and information errors by a factor of 4 and demonstrate improvement in teamwork
Despite being really pleased with these outcomes, the work proved quite difficult to publish, eventually emerging in a small circulation Pediatric Anesthesia journal. The medical literature remains fonder of genes, drugs and new operations than of papers concerned with process. However, after presenting the work in the USA, the findings were picked up by the Wall Street Journal, reaching an audience of millions
3, and we found ourselves being asked to speak about what we had learned in company boardrooms and hospitals throughout the world. Handovers between teams are common in all industries and indeed occur at every shift change, and everywhere were a focus of increased risk. The structural approach we had learned from F1 clearly had relevance everywhere, and indeed remains so.
These processes and formalized team working are now in use in medicine throughout the world, and the success has been replicated. It is now core business.
Several thematic lessons are important.
Firstly, there is no substitute for Standard Operating Procedures (SOPs) for repeated tasks. It is too easy for a team that works together regularly to take short cuts and miss out some key step. One individual member can assume the other has done their job, (because they always do their job, don't they?) only to discover later that they did not, because on this occasion they forgot. Checking everything avoids that, hence structure and checklists.
Secondly, understanding and respecting everybody's role is critical, otherwise you get in each other's way. There is probably no worse place to have a cardiac arrest than in a room full of doctors….they will all try and help!
Thirdly, recognizing the importance of rehearsal. Medicine has proved itself to be quite good at analysing adverse events after they have happened. It has been less successful in undertaking repeated rehearsal until everybody gets it right every time. As Peter Van Manen, an ex-McLaren engineer, put it to me, "80% of what happens in a hospital is completely predictable. Good SOPs should make them reliable. That would free the intellectual capacity of the staff to sort out the vital 20% that is unpredictable".
Fourthly, embedding the routines in daily life with frequent retraining.
Fifthly, and perhaps most relevant to the world of paediatric cardiac surgery, an absolute, individual commitment to excellence….because the baby we operate on is a precious gift, simply loaned to us for care by doting parents.
By analysing and modifying an apparently simple process by applying the lessons from F1, we were able to make great improvements in the quality of our teamwork. Cardiac surgery in the modern era is all about teamwork, and getting that right is a crucial goal.
The relationship between healthcare and F1 has not been a one-way street, and I want to take a moment to consider what medicine has done for them. Obviously, we were able to teach the pit crews about some important new techniques which would be of value to them. And our prenatal diagnostic techniques have helped them with identifying new talent.
This reciprocity is also evident in the second important domain in which F1 has exerted influence over health care. That domain is safety. Since F1 began around 1950, it has been self-evident that it is a dangerous sport, both to spectators and drivers, and fatalities were frequent amongst both in the early days. In the early days, there were no seatbelts, little in the way of driver protection, and nothing to retain parts of the cars if they crashed. Speeds were high, fuel was highly inflammable and leaked on impact, and even the alloys used to build the car were flammable at high temperature. Just look at this clip of the famous Le Mans race of 1955 (www.youtube.com/watch?v=j0RfHIjgr0c), which whilst not from F1, makes the point very clearly. Good medical care was needed for both drivers and spectators, and the knowledge and skills of medical personnel have had a significant impact on the safety of F1. Undoubtedly the most notable contributor to safety in F1 is Professor Sid Watkins4 5. Watkins was a self-confessed lifelong petrol head and bon viveur, but also a highly renowned and well connected neurosurgeon.
Watkins started to work in F1 in the early 1970's as a doctor at Watkins Glen when he was working in the USA. He became more directly involved in F1 in 1978 and was immediately involved in dealing with some of the most infamous accidents in the business. His neurosurgical knowledge, resuscitative skills, scientific objectivity and awareness of car design made it possible for him both to catalogue the types and causes of injuries that happened to drivers, but also to work with designers to make the cars safer. We have moved from an era in which the driver could be flung form the car or incinerated in it to one in which the car, even crashing at very high speeds, actually protects the driver. It has been a remarkable transition.
Sid Watkins personality generated excellent relationships with drivers and teams alike, and with the commitment of Bernie Ecclestone resulted in a huge and successful push to make F1 safer. They succeeded. Since 1994 there has only been one death in F1, that of Jules Bianchi at Suzuka in 2014. He was going rather fast even behind the safety car for the appalling weather and hit a recovery vehicle, which was inside the barriers. F1 cars have open cockpits….for the time being.
What this history demonstrates is importance of having a total, systemic, commitment to safety. This commitment has been replicated in several industries, for example railroads, nuclear and airlines, making them high reliability organisations. Anyone who has visited a major construction site in the last year will recognize the improvements that have been made in that industry in the last decade. Medicine could and should do that too, but we have been much less effective in implementing the necessary changes across health systems.
Many of the safety features and technical innovations found on F1 cars have found their way into our own road cars. F1, and motorsport in general, has thus improved road safety..although you could argue that they (and Top Gear) also encourage people to think they can driver like Lewis Hamilton.
These contributions to road safety have reduced fatalities, and the frequency and severity of injury but paradoxically reduced the number of available organs for transplantation, which has implications for other of my patients. Despite this, I still regard the advances in road safety to be of greater importance.
The next domain of benefit from F1 that I want to discuss is the collection and analysis of large amounts of data. F1 is very much a data-driven sport. Everything about the car and its performance, from aerodynamics to engine temperatures and tyre performance, is monitored and analysed. The data collected are used to change strategy, inform tactics and to redesign the car, week by competitive week. Ross Brawn, the renowned F1 team manager, has said that Formula 1 is really "an annual engineering competition. You build a new car in the closed season, and continuously modify it during the season". The rate of change in F1 cars during the season is astonishing6, and none of it would occur without data to support and justify the investment needed to make a design or strategy change.
Each car, whilst being built to a specific design and specification, does turn out to behave differently and individually during each race. This is very much like the varied 'performance' of our patients in the ICU. They may be the same age, have the same diagnosis and have had the same operation, but their individual performance is different. The F1 teams accumulate masses of data not only to monitor performance but also to predict when problems might occur. We monitor our patients using several parameters, for example pressures in arteries and veins, oxygen saturation, temperature and so on, but we are largely reacting to what we see, rather than predicting what might happen. To be able to intervene before something bad happens is the holy grail of intensive care, but has proved very difficult to achieve in real life.
Modern Formula One cars are very much more closely monitored than our children in the operating room or in ICU. In race trim, there are about 125 sensors sending data on 500 different parameters generating about 13,000 'health' parameters relating to the car. These data are sent back to the engineers in the pits at a rate of 2-4 MB/sec and thence back to the base factory (usually in another country), monitoring the function of a variety of components from the engine, the suspension, to tyres and various gas flows. This amounts to 750 million numbers in a two-hour race. In qualifying, there may be even more, up to 300 sensors, and a variety of cameras watching key components, especially tyres. These various information sources result in a massive amount of data 7 being collected for analysis. During the US grand prix in Austin last year, the teams collected a total of 243 terabytes of data, more than contained in the entire US Library of Congress in Washington. The data are monitored and analysed by 10's of specialists, turning data into knowledge and adding insight, suggesting the changes to improve performance and reliability.
These data flows create massive data sets…spreadsheets with hundreds of columns of potentially interacting variables. Understanding how these variables interact is essential to separating what really matters from the noise of the data.
These graphical representations of data, wiggly lines on a screen, bear a clear resemblance to the waveforms seen on the monitoring screen devoted to a baby in ICU. I have already described that each baby is different, and behaves differently in response to intervention the clinicians might feel they need to make. The very fact that a baby is in ICU means that its measured values are not 'normal', but they may be normal for a child in those circumstances. Wouldn't it be great if we could use similar data analytic tools to those employed in F1 better to understand what is causing perturbations in monitored values or to predict what is about to happen to a child? Well, this has begun to happen.
McLaren Applied Electronics provide much of the data acquisition systems for F1, including the Electronic Control Unit present in all cars. They have begun to work with Birmingham Children's Hospital to apply their expertise in F1 to the very sick babies in ICU. I have the privilege of being able to share some of that work with you tonight, and I do so courtesy of Heather Duncan, consultant intensivist at BCH, Peter Van Manen who was working with McLaren when the project was established, and the entire team at McLaren notably Caroline Hargrove, Duncan Bradley, Adam Hill and Ian Rhodes.
In most hospitals, the data from the wiggly monitoring lines of an individual child are stored for less than 48 hors, if at all. Mainly they are used for real-time monitoring. McLaren have made it possible for Birmingham to store much more data over longer periods, allowing the data to be analysed at leisure and subjected to Principal Component Analysis, a statistical technique which allows the components of change to be separated and the components plotted against each other. Here a 'cloud' of normal data is shown in green, collected over about 30 minutes. When significant changes occur, as the wiggly lines on the monitor change, the visible data deviates away from the 'normal' cloud. For simplicity, further period of data collection associated with abnormal values is coloured red, highlighting significant variation, which itself could be predictive in future. Of course, the green area may not be an 'ideal' state, and the red may represent an improvement. Human assessment, by clinical observation, is still needed to provide that insight, at least at present. The data presented look not just look at the amplitude of change, but by the use of PCA at the history of change. The plots produce cues that important change may be taking place and can focus the minds of the attending team. As more data are accumulated on more and more patients are studied, and as more and more patterns emerge, then the potential for the application of artificial intelligence for decision support is clear.
Other solutions are available. At Boston Children's, Toronto Sick Kids and Great Ormond Street we are using another system, which is trying to do the same thing. This system is called T3 and was developed with Etiometry ( http://www.etiometry.com/t3/) and NASA.
Both systems will be able to accumulate and analyse considerably more data than ever before. The more data we have, the more we should learn. Both systems will also benefit from developments in wearable sensors and improvements in transmission of data, which will move data analytics out of ICU and into real life situations. There are several diagnoses and procedures in cardiac surgery that require very close supervision of children at home, by parents and nurses alike. For example, between the 1st and 2nd stages of surgery for hypoplastic left heart syndrome, it is vitally important to monitor oxygen saturation, pulse rate and weight. As physiologic sensors develop (as the physical sensors in F1 developed), then monitoring of children at home and applying data-based algorithms to suggest appropriate therapies will become reality and children may need to spend less time in hospital, both improving quality of life for them and freeing up capacity for us.
I see these developments having widespread and potentially disruptive significance in medicine. What we will learn from these early studies will help us to develop methods to manage a wide range of other diseases, and to apply increasingly precise models to guide our decision making. We will collect further evidence from many patients, each time learning from the preceding intervention.
Even within the domain of big data, teamwork and personalities are important. When I spoke to Peter Van Manen about the work at Birmingham, he made some very important points about what makes a center able to innovate. Despite what it may seem, the environment of a modern children's hospital is significantly more complicated than that of Formula 1. Our teams are not always the same, indeed they are often ad hoc, even on a daily basis. And whilst all F1 teams are different, with different personalities and team characteristics, much of the base equipment, for example the electronic control unit in the cars is standard, providing a platform on which the individual teams can build.
The hard work, he said, was establishing the right culture in the first place. The necessary culture is characterized by self-criticism, a willingness to learn and a willingness to change based on the data obtained. He praised Dr. Heather Duncan for the groundwork she had done at Birmingham, particularly in leading work on early warning systems in intensive care.
Happily for us he also observed that people working with children were generally extremely committed to innovation and had a good culture of sharing information. To make some of the decision doctors who care for children have to make you need courage, and especially so if the information available to you is limited or even not available. Some risk has to be taken to do what we do, and the decision to do nothing is equally important. The advantage of the collection of large amounts of data on every child is that such decisions can be analysed and future choices simplified or improved.
Whilst the current gold standard research tool in medicine is the randomised controlled trial, (in which a selected group of patients is randomised to receive one or other therapy and monitored against defined outcome criteria to determine which treatment is better), these big data analytic tools will provide an alternative and perhaps more appropriate tool for studies in complex, heterogeneous groups of patients like ours. I am very glad that McLaren, Etiomery, NASA, SAS, IBM, and many other big companies are getting into the healthcare market. There is much to learn.
The data that are collected in F1 not only provide predictive analytics for strategy and tactics, but also feed a system of rapid development, prototyping and application that is the envy of those of us who work in healthcare. This is the next domain of learning from Formula 1 I wish to cover. There are about 25,000 components in the average F1 car, and during the season, after the car has been designed and built, multiple changes take place to those components. Every two weeks about 5000 new components are manufactured to fit to the car to try and make it go faster. 5 to 10% of the car will be different every two weeks of the year. To get some idea of what those changes are have a look at this website;- http://www.formula1.com/content/fom-website/en/latest.html?type=Technical. The car might look largely the same, but in reality is quite different at each race.
The design and redesign of these components is based on the data obtained from the cars in practice and during the race. The processes are effectively continuous. The rate at which development has to occur places huge demands on the system. The advent of computer aided design (CAD) together with 3D printing and new materials has changed things considerably, making rapid prototyping and manufacture a reality.
F1 has led the way in the use of 3D printing both to create models of cars and components to test aerodynamics in the wind tunnel (where testing is limited to 60% scale models), but also rapidly to make components for the car itself, for example ducting and some titanium components. Printing machine size and current strength and the cost of materials [1] limits the use, but all that will change with time. This rapid turnaround of idea, design and testing is the basis of F1.
How wonderful it would be to be able for us in surgery to turn around an idea for an improved piece of kit within a week, as is often done during the season in Formula One. The transition from idea to product in health care, certainly in the UK, is so laborious that many people give up at stage one. We need to build a much more responsive development system if we are to maximize the intellectual potential of our staff, and we are beginning to see examples of that in practice, for example printing new instruments for testing (or even direct use), rehearsal of procedures or theorizing about modes of repair. The relationship between hospitals, universities, industry and investment capital is being revised, and there are several successful examples of how such innovation is happening, for example in Stanford and Georgetown Universities in the USA, Helsinki in Finland and in the UK at UCL, Imperial and Cambridge.
With rapid prototyping comes rapid failure; the need to recognize an idea which is not working, and move on without regret. My experience of hospitals and universities is that, largely, they don't get this idea. Yet they must begin to do so if the good ideas amongst the pack are to be developed. However, I think the NHS remains a bit behind the game, largely because of risk aversion or fear of early adoption.
This rapid turnaround of ideas to create multiple small improvements in performance is not confined to F1. It describers the fashionable theory of 'marginal gains', a theme later developed by Dave Brailsford with the British Cycling Team and emphasised again in Matthew Syed's new book, Black Box Thinking 8. Hospitals like GOSH, Birmingham Children's Boston and Toronto contain elite teams, which can and do apply these methods as far as they can. Indeed, over the last 60 years cardiac surgery for children has become a lot safer, and we have become able to manage a wider range of conditions than thought possible at the start. Much of that progress has been made by multiple iterative steps, amounting to a process of continuous improvement sometimes called Quality Improvement, rather than conventional randomized trials. QI is applied in many industries and many sports. However, I doubt if all industries, motor racing teams, cycling clubs and table tennis clubs can apply marginal gains effectively any more than healthcare has been able to. You still need that core culture which supports and fosters innovation. And you need a motivated work force with clear goals. At Great Ormond Street, I have had the privilege of working in such an environment, but even there proven successful techniques developed in one area are extremely hard to get adopted in another. And it is even harder to get successful ideas embedded in other institutions. People are distrustful of change initiated elsewhere (especially if developed in a prestigious place), and prefer their own ideas. Spread is difficult to achieve, and there are so many ideas that you might wish to adopt.
We have also learned from the study of aerodynamics in F1. With colleagues at Imperial College, UCL and Great Ormond Street we have applied 9 similar flow dynamic modeling to 3D datasets of the trachea to monitor disease progress in children, which we can now do without having to pass a telescope down the trachea or give an anaesthetic. My colleagues in craniofacial surgery, led by MR. David Dunaway, have also used similar surface scanning technologies to those used by Williams to purpose fit helmets to drivers to plan surgery and with 3D reconstruction and printing to develop personalized procedures and parts.
There are several good examples of products, directly developed from F1, making it into the health care sector. The monocoque construction of the drivers safety cage, and the use of ultra-lightweight materials have been adapted by former F1 engineer, Mike Spindle ( http://www.trekinetic.com/) , to create the wonderful Trekinetic Wheelchair, which has front wheel drive, active braking and nitrogen suspension.Another good example, developed by Mike Lait, is the Babypod (http://www.babypod.com/) , a transport incubator to make moving sick babies safer, and easier. The Babypod is <10% of the weight of a conventional incubator, and fits easily into most modes of transport.
The complexities of transport leads me neatly to the final domain I want to mention is that of logistics. This is an area just beginning to be explored between our two worlds. At least every two weeks during a season, each F1 team has to move 90 tons of equipment including spares and tools, 2 or 3 cars and all the supporting people around the world. Everything and everyone must arrive safely, be accommodated, be fed and watered and be able to work. And the IT has to work. Yet is hard to imagine a team ever being late! And the race always starts on time. Teams outsource their logistics to companies such as DHL, but these repeated successful journeys of precious cars, drivers and engineers around the world can surely teach us a thing or two about how we can get our precious patients through the byzantine pathways of hospital care, and how to get our operating lists and clinics to start on time.
We are beginning to work with F1 on exactly these problems, and working out exactly what data we need to collect to monitor these patient journeys and find and correct rate-limiting steps. Throughout the world, getting operating lists and clinics to start on time remains a challenge, and health IT is notorious. Our resources may be limited, our scale small, but there are many of us around the world, and if we can obtain good data make our processes and logistics better we should be able to help more people for lower cost and still get great outcomes. What is not to like about that.
Conclusion
The motivation and clarity of purpose that is necessary to succeed in Formula One was eloquently described by Ross Brawn at a recent Risky Business conference 10. The purpose of having a team in F1 is to win. Every part of that team, every member, must be the best at what they do in Formula 1. Every activity they do must be the best. Each person must know what they need to do to become the best and each one must be set tangible personal objectives that relate to that overall strategy of excellence. Formula One is always about managing a crisis, and to manage that crisis the members of the team must give them the tools and the resources to do so. The team principal must work out what needs improving, and determine the things that need to be done. Brawn found it effective to build little teams within the big team to stimulate competition, but ensure that individual success was not achieved at the expense of others.
In F1 it is easy to see which team is best. 100 million people can see that at every race. And there is only one end-point, one bottom line. Victory. Understanding which team is best in cardiac surgery is much harder, as there are so many outcomes that might be judged as successful depending what values the family uses. But excellence will require us to know our performance and to be able to identify who is best in class. The gap between one's own team and that best in class team should be bridgeable, bringing up the quality and performance everywhere. There is nothing to be gained from pursuing measures relating to the national average performance; being better than average is not good enough if you want to achieve excellence.
I have been privileged to work in a unit where that has been the ethos for decades. It has produced both quality and innovation, and I am proud to have been a member of the Great Ormond Street Children's Hospital team. It is all about teamwork, as the motto of STRAKA Racing says; " talent wins races, but teamwork and intelligence win championships".
Further reading
1. de Leval MR, Cart hey J, Wright DJ, et al. Human factors and cardiac surgery: a multicenter study. J Thorac Cardiovasc Surg 2000;119(4 Pt 1):661-72.
2. Catchpole KR, de Leval MR, McEwan A, et al. Patient handover from surgery to intensive care: using Formula 1 pit-stop and aviation models to improve safety and quality. Paediatr Anaesth 2007; 17(5):470-8.
3. Naik G. A Hospital Races to Learn Lessons of Ferrari Pit Stop. The Wall Street Journal 2006 14 November 2006.
4. Watkins S. Life at the Limit: triumph and tragedy in Formula 1. London: Macmillan, 1996.
5. Watkins S. Beyond the Limit. London: Macmillan, 2012.
6. The Latest in Formula 1. Secondary The Latest in Formula 1 2015. http://www.formula1.com/content/fom-website/en/latest.html?type=Technical.
7. Bi F. How Formula One Teams Are Using Big Data To Get The Inside Edge. Forbes. New York: Forbes, 2014.
8. Syed M. Black Box Thinking: the surprising truth about success. London: John Murray, 2015.
9. Hamilton NJ, Kanani M, Roebuck DJ, et al. Tissue-Engineered Tracheal Replacement in a Child: A 4-Year Follow-Up Study. Am J Transplant 2015; 15(10):2750-7.
10. Brawn R. What it takes to win the F1 Championship. Secondary What it takes to win the F1 Championship 2012. http://www.risky-business.com/video.php?videoid=110.
I may be old enough now to be in a museum. But being part of a museum exhibition was not something I expected to do in my lifetime, but these developments with F1 did find their way into the Science Museum as part of an exhibition called "Fast Forward". You can see a summary of that exhibition here, presented by the curator ( https://www.youtube.com/watch?v=qNVWe-86saA).
Paediatric cardiac surgeons have been at the forefront of monitoring their own and their team's performance and have been publishing their data publicly for decades. If you are interested, you can explore current UK results at this website; https://nicor4.nicor.org.uk/CHD/an_paeds.nsf/vwContent/home
Acknowledgements
There are so many people to thank for their help in both the work we have done with F1 over time and in the preparation of this talk. It has been a real honour to work with them.
Firstly, I would lick to acknowledge the inspiring contributions of Professor Marc de Leval, Professor James Reason, Captains Guy Hirst and Trevor Dale who stimulated our interest in safety and human factors, and the research conducted by Dr Jane Carthey. Secondly, Drs. Allan Goldman and Angus McEwan at GOSH who helped drive the research into the application of pit stop methods. Dr Ken Catchpole, now in the USA, actually carried out the pit stop research with Annette McQuillan, but we would not have been able to do it at all without the late Professor Sid Watkins, Ron Dennis of McLaren, and Ross Brawn then with Ferrari working with the late Nigel Stepney.
More recently, I am grateful to the entire team at McLaren Applied Technologies, namely Ian Rhodes, Caroline Hargrove, Duncan Bradley and Adam Hill. They have been generous with time, views, energy and images…and my race suit. I will never forget sitting in their race simulator. I look forward very much to our developing institutional research partnership.
Clare and Frank Williams at Williams F1 were incredibly generous with time and experience and it was a privilege to tour the museum there with Sir Frank and to see the manufacturing of F1 components.
Dr. Heather Duncan at Birmingham Children's Hospital and Peter van Manen, formerly of McLaren, provided data and images and important insight and explanations. Professor Peter Laussen of Toronto Sick Children discussed T3 with me.
© Professor Martin Elliott, 2015
[1] In 2014, the cost of a resin refill for a typical F1 3D printer was in the order of £60,000…still much cheaper than going straight to labour intensive carbon fibre.
Part of:
This event was on Wed, 14 Oct 2015
Support Gresham
Gresham College has offered an outstanding education to the public free of charge for over 400 years. Today, Gresham College plays an important role in fostering a love of learning and a greater understanding of ourselves and the world around us. Your donation will help to widen our reach and to broaden our audience, allowing more people to benefit from a high-quality education from some of the brightest minds.


 Login
Login